

Case:
- A 32 year old woman presented with experiencing painful debilitating daily migraines for the past 8 years.
- The pattern of migraines started in the morning and built throughout the day until they become debilitating and each day the patient would have to go to bed. The patient complained of Aura style headaches and a building of pressure within the head to the point where she had to lie down in the early evening to alleviate the pain.
- The patient had been to their GP and subsequently refereed to a consultant and told that there was nothing that could be done for her and given migraine medication which she became dependent on to manage the symptoms.
- The patient was told by a friend to try osteopathy and see if that could help.
- Having gone through the case history with the patient it became clear that the patient suffered a severe Road Traffic Accident 8 years previously. The patient was stationary at a roundabout and was hit at speed by a car from the rear suffering whiplash. After the accident the patient had a short course of physiotherapy and was told that all was resolved.
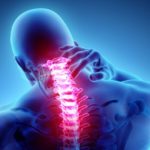
- However, the patient had 3 osteopathic treatments which focused on releasing the joints at the base of the skull along with releasing joint restrictions through the cervical spine, thoracic spine and upper ribs to resolve the migraine issue.
- The patient’s migraine problems were completely resolved post treatment and the causation was the structural biomechanics of the spine and skull affecting the blood pressure into and out of the skull.
- This explained the building up of pain and pressure throughout the day into the patients head and the symptoms being alleviated from the patient having to lie down.
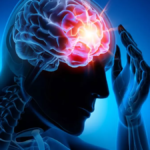
What Is A Migraine?
Migraine pain is an intense pulsing, pounding , throbbing from deep within your head. The exact cause of migraines is unknown, but they’re thought to be the result of abnormal brain activity temporarily affecting nerve signals, chemicals and blood vessels into and out of the brain.
Restricted joints in the upper back and into the neck (cervical spine) can also cause pressure migraines which are a result of increased internal pressure within the skull and then onto the brain.
Migraine Triggers
Many possible migraine triggers have been suggested, including hormonal, emotional, physical, dietary, environmental and medicinal factors.
These triggers are very individual, but it may help to keep a diary to see if you can identify a consistent trigger.
It can also sometimes be difficult to tell if something is really a trigger or if what you’re experiencing is an early symptom of a migraine attack.
Physical triggers:
- tiredness
- poor-quality sleep
- shift work
- poor posture
- neck or shoulder joint restrictions
- jet lag
- low blood sugar (hypoglycaemia)
- strenuous exercise, if you’re not used to it
Medicines:
- some types of sleeping tablets
- the combined contraceptive pill
- hormone replacement therapy (HRT)
Emotional triggers:
- stress
- anxiety
- tension
- shock
- depression
- excitement
Environmental triggers:
- bright lights
- flickering screens, such as a television or computer screen
- smoking (or smoky rooms)
- loud noises
- changes in climate, such as changes in humidity or very cold temperatures
- strong smells
- a stuffy atmosphere
Dietary triggers:
- missed, delayed or irregular meals
- dehydration
- alcohol
- caffeine products, such as tea and coffee
- specific foods, such as chocolate and citrus fruit
- foods containing the substance tyramine, which include cured meats, yeast extracts, pickled herrings, smoked fish (like smoked salmon), and certain cheeses (such as cheddar, stilton and camembert)
Hormonal changes:
- Some women experience migraines around the time of their period, possibly because of changes in the levels of hormones such as oestrogen around this time.
- These type of migraines usually occur between 2 days before the start of your period to 3 days after.
- Some women only experience migraines around this time, which is known as pure menstrual migraine.
- But most women experience them at other times, too, and this is called menstrual-related migraine.
- Many women find their migraines improve after the menopause, although the menopause can trigger migraines or make them worse in some women.
How Long Do Migraines Last?
They can last from 1 minute, to 4 hours to a few days and significantly limit your ability to carry out your daily routine.They usually happen one to four times per month but can quite often occur daily and often show no consistent pattern of occurrence.
Along with the pain, people have other symptoms, such as sensitivity to light, noise, or smells; nausea or vomiting; loss of appetite; upset stomach or belly pain, panic attacks and irritability.
Some migraines are preceded by visual disturbances and about one out of five people will experience these symptoms before the headache starts. These are known as an ‘Aura Migraines’.
They may cause the patient to see:
- flashing lights
- shimmering lights
- zigzag lines
- stars
- blind spots
‘Aura Migraines’ can also include tingling on one side of your face or in one arm and result in the patient having trouble speaking which may lead some others to believe the patient is in fact drunk.
However, the symptoms of a stroke can also mimic a migraine.
If any of these symptoms are new to you, you should seek immediate medical attention.